I’M TICKED OFF!
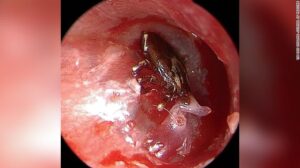
Like some of you, I read the incredible story that broke several weeks ago about the 9-year-old little boy in Connecticut who had a tick embed itself in his eardrum. According to a report in the New England Journal of Medicine co-authored by Dr. Erik Waldman and Dr. David Kasle 3 days before the boy was brought to the Yale-New Haven Children’s Hospital, he had been hearing a very faint buzzing in his right ear as he played outdoors at his school.
Susan Scutti of CNN originally wrote the story on May 1st of this year, if you haven’t read it check it out, but that’s not why I’m ticked off, you see after reading that incredible and freighting story you would think that I would have been on high alert for ticks the rest of the summer or at least for the next few weeks right?
SO WHY AM I TICKED OFF?
Well, you never think it’s going to happen to you until it does and then you ask yourself “why me”. In this case, the answer is quite simple, I’m a dummy! As someone who has been working in the outdoors shooting the Fish’n Canada Show for almost 40 years, I should be the last person on earth to go trouncing around the woods without taking proper precautions against ticks. Well like I said, some of us are just plain dumb and that’s why I’m ticked off!
WORKING IN THE FIELD
I was recently out in the Long Sault Parkway area of Ontario marshaling a fishing event, the Fish’n Canada Carp Cup, and although I wore long pants and long sleeves, I didn’t spray myself with a repellent containing permethrin or deet, the only known chemicals that repel these nasty little parasites from hell called black-legged ticks also known as deer ticks. By now you’ve probably surmised, I became a host for this evil bloodsucker and consequently may have exposed myself to Lyme Disease. To make a bad situation even worst, my 16-year-old grandson Niki, who was with me at the time, may also have become infected. I say may have, because not all ticks are vectors for this relatively new scourge of humanity. However, according to Public Health Ontario, the risk areas in the province are rapidly growing each new year with the latest Hot Spot being, you guessed it, the Long Sault, Cornwall, Ottawa area. Most of the provinces are now reporting ticks at levels of concern. There is a great story on Global News website called Tick-Tock you should check out.
THE SOONER THE BETTER
After carefully removing the ticks, thanks to some really good removal information on WebMD.com, Nik and I decided that when we got back home we’d go in for the Lyme disease test however we weren’t going to wait for the results but rather, go on the 21 day treatment program as outlined by the CDC Centers for Disease Control and Prevention and not take any chances. I suppose some of you may think that this course of action might be a little extreme but let me fill you in on some hard facts. First of all, according to most of the experts, the current test methodology has a 50/50 chance of being accurate on the first result, so much so that when you go in to have the test done they automatically schedule you in for a second test 10 days later. If both tests come back identical then the result is confirmed, however if both tests come back different then a new test is ordered 10 days after that, then it becomes a best two out of three series, they take the 2 identical test results as being accurate and throw out the bad one but even so, apparently there is a 20% chance that they’re still wrong. Meaning that by now almost 30 days have gone by since you were originally infected, and you still might not be properly diagnosed. The real concern here is according to the experts, the longer you wait to start treatments the more difficult it becomes to cure, in fact, most of the science says that the first 24 to 48 hours are critical. I don’t know about you but for Nik and me, it was a no brainer, 21 days of popping piles or a possible lifelong debilitating disease, pills it is.
THE FIRST MEDIA OUTLET TO TALK LYME
As host of Outdoor Journal Radio, I have been closely following the Lyme disease story for the past 15 years or so and interviewed countless people who have been studying, diagnosing, treating and lecturing on this enigma scientifically know as Lyme borreliosis. As well, some of our guests have been people who had various levels of the infection, from freshly diagnosed positive to Katherine Maroun host of “What a Catch” television show who had been battling with Lyme for over 10 years. You can hear the interview on ODJRADIO.
DO AS I SAY NOT AS I’VE DONE
All of this to say I should have known better but I didn’t, I let my guard down and now I’m hoping that this message will resonate with anyone who is exposed to the outdoors to take the precautions that are well documented on the Government of Canada’s Surveillance of Lyme disease, National Collaborating Center of Infectious Diseases, Public Health Ontario, E-tick.ca. All of these sites have a wealth of information on how to prevent, how to diagnose and how to cure Lyme disease and even how to properly remove ticks. Please use this article as a wakeup call. Don’t be a dummy like I was, be smart and enjoy the outdoors for years to come. In other words, do as I say not as I’ve done.